£299.00

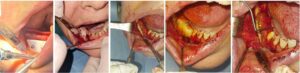
1. Iimori Y, Kameshima Y, Yasumori A, Okada K. Effect of solid/solution ratio on apatite formation from CaSiO3 ceramics in simulated body fluid. J Mater Sci Mater Med 2004;15:1247–1253. 2. Xu S, Lin K, Wang Z, Chang J, Wang L, Lu J, Ning C. Reconstruction of calvarial defect of rabbits using porous calcium silicate bioactive ceramics. Biomaterials 2008;29:2588–2596. 3. Hing KA, Wilson LF, Buckland T. Comparative performance of three ceramic bone graft substitutes. Spine J. 2007; 7(4):475-490 5.Dashnyam, K.; El-Fiqi, A.; Buitrago, J.O.; Perez, R.A.; Knowles, J.C.; Kim, H.-W. A mini-review focused on the proangiogenic role of silicate ions released from silicon-containing biomaterials. J. Tissue Eng. 20 17, 8, 1–13. 7. Licina et al, Comparison of (SiCAP) with (Infuse) in Posterolateral Instrumented Lumbar Fusion Global Spine J 2015;5:471–478. 8. Khoury F. (2017) Augmentation of severe bony defects with intraoral bone grafts: biological approach and long-term results. http://dx.doi.org/10.1016/j.ijom.2017.02.099